
How published research can shape scaffolded learning for safer prescribing
30 April 2026
How published research can shape scaffolded learning for safer prescribing
This post reflects on how two strands of published research on medicine safety were used to design scaffolded learning for safer prescribing. Drawing on work in pharmacovigilance and pharmacogenetics, it shows how research can be translated into case-based learning that helps learners interpret uncertainty, discuss medication-related risk clearly, and make more reasoned prescribing decisions in practice. It also offers a practical example of how published evidence can become something learners actively work with rather than something they simply read.
Published research often ends up as something learners read about rather than something they actively work with. We wanted to do something different. We took two strands of our published work on medicine safety and used them to design a linked, scaffolded set of workshops for safer prescribing. Rather than asking learners simply to absorb evidence, the teaching focused on how they interpret uncertainty, communicate risk clearly, and respond when medicine-related harm is suspected in everyday clinical practice
Our example came from pharmacovigilance and pharmacogenetics. (In brief, pharmacovigilance is how we keep watching the safety of medicines after they are in real-world use, and pharmacogenetics is the study of how a person’s genetic differences can affect the way they respond to medicines.)
However, the teaching point is broader than those subjects. The real challenge was not simply how to explain the science. Our goal was to:
• Begin with a real prescribing problem and the evidence needed to think it through
• Use realistic cases to keep the teaching close to clinical practice
• Help learners to weigh evidence and make reasoned decisions when the answer is not straightforward
Start with the teaching problem, not the paper
Our starting point was a familiar challenge in health professions education. Medicine safety matters enormously, but it can easily feel abstract when it is taught mainly as a reporting process or a list of cautions. Learners may remember the content but still feel unsure about how to use it in an actual prescribing decision.
That shaped the design of the first workshop. We used selected Safety Charts derived from our open-access comparative safety analysis to help learners compare medicine risks by viewing side effect reports alongside prescribing volume. Readers who would like more detail on the underlying research can find the Safety Charts in our paper here. The aim was not simply to present our published work. It was to build a practical teaching sequence around a real question: how do we compare medicines regarding risks and discuss risk when the evidence is imperfect?
We also stressed that Safety Charts should support, not replace, clinical judgement. That mattered educationally because it encouraged a more critical use of the available evidence. Case-based discussion became central; rather than treating pharmacovigilance as a compliance topic, as it is so often taught, we used realistic scenarios to help learners recognise its limits and explain risk in practice. This changed the nature of the session. It became less about memorising information and more about applying the available evidence to real prescribing decisions.
Design scaffolded learning, not a standalone session
One of the most useful design choices was to think in terms of sequence rather than separate teaching events. The first workshop focused on how medicine safety signals are recognised and interpreted in real-world data. That led naturally to a second question: why do some patients experience harm while others do not?
That question became the basis of the follow-on workshop, where we introduced pharmacogenetics as a second lens on individual risk. Importantly, we did not present this as a separate specialist topic. We kept pharmacovigilance at the centre and used pharmacogenetics to extend the original discussion. That mattered because it helped learners see connections rather than experience the topics as isolated blocks of content.
We first re-established pharmacovigilance as part of everyday prescribing, then introduced pharmacogenetics as another way of thinking about why medicine response may differ between patients. This kept the focus on safer decision-making rather than technical detail for its own sake.
Keep the science, but simplify the learning task
A second lesson was that published research needs translation before it becomes teachable. In the second workshop, baseline responses suggested that familiarity with both pharmacovigilance in routine practice and pharmacogenetics was very limited. We therefore had to keep the learning task simple, even though the underlying science was not.
In practice, that meant structuring the session around a small set of questions:
• What does the available evidence suggest?
• What are its limits?
• How would you explain the medicine-related risk?
• What action would you take?
These questions made the teaching more usable because they gave learners a structure for reasoning under uncertainty.
What other educators can take from this
For us, the wider lesson is that published research should do more than sit behind a lecture or reading list. It can become the backbone of scaffolded learning when learners are asked to do something with it. In our case, that meant moving from published research on medicine safety to a practical prescribing problem, then to case-based workshop discussion, and finally to action in practice.
Although our example sits within medicine safety, the same principle applies much more widely. Across disciplines, teaching becomes more engaging when published research is used to frame a practical problem and help learners work through uncertainty rather than avoid it. That is what made these workshops effective. The research mattered, but its educational value emerged when learners were asked to work with it, question it and use it.
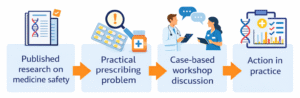
Image source: https://coreprescribingsolutions.co.uk/pharmacogenomics-personalised-medicine/
Further reading
- Mokbel, K., Daniels, R., Weedon, M.N. and Jackson, L. A comparative safety analysis of medicines based on the UK pharmacovigilance and general practice prescribing data in England. In Vivo. 2022. DOI: 10.21873/invivo.12765
- Mokbel K, Weedon M, Daniels R, Moye V, Jackson L. Evaluating genotype-treatment interactions for high-risk medications in British general practice: a retrospective cohort study using UK Biobank. British Journal of General Practice. 2026. DOI: 10.3399/BJGP.2024.0806
For more information please contact:
This post was written by Dr Kinan Mokbel and Dr Rob Daniels, University of Exeter.

